What Is an Ostomy Reversal?
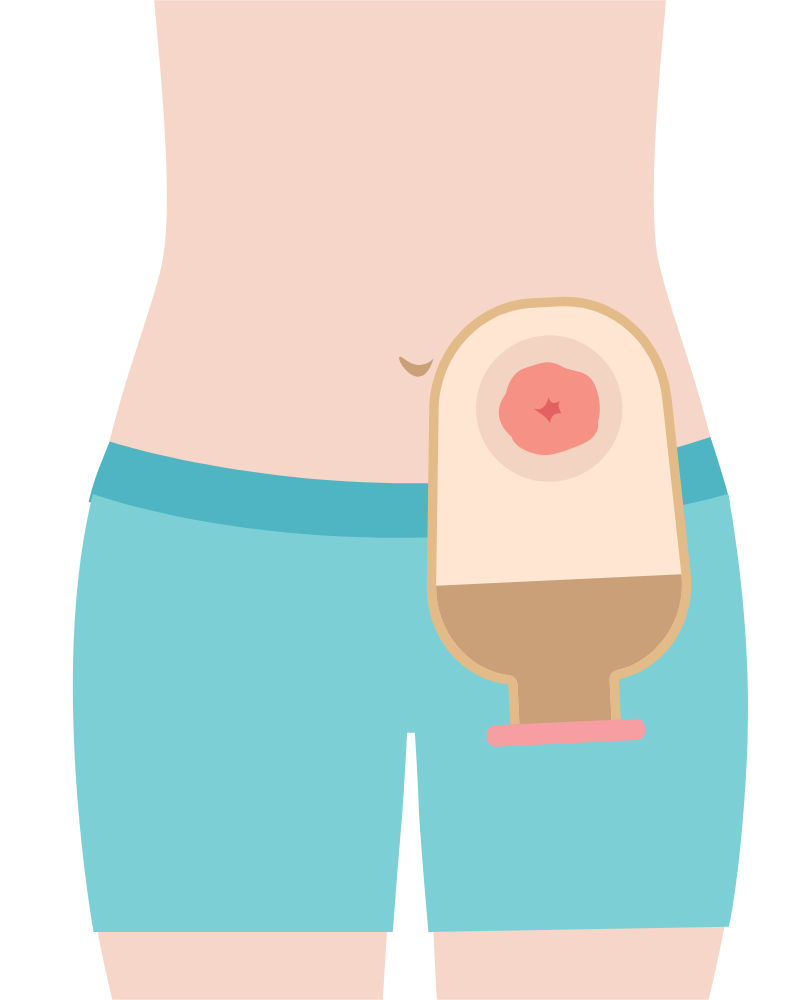
First, what is an ostomy?
An ostomy is a surgically created opening (a stoma) on the abdomen that allows urine or stool to exit the body when the natural pathway is blocked or damaged, rerouting waste into an external pouch.
Common types include colostomies (colon), ileostomies (small intestine), and urostomies (urine), often needed for conditions like cancer, inflammatory bowel disease (IBD), or injury. These may be temporary, or permanent.
Our website focuses on the reversal of a colostomy or ileostomy.
Colostomy Vs. Ileostomy
These two types of ostomies are quite different. While both are diversions of the normal digestive process, they occur at different parts of the body.
- Ileostomies are placed in the small intestine, or ileum. They are ‘higher up’ in the digestive system, and are often used when the large bowel that is ‘lower down’ needs to heal. Ileostomies are typically on the right side of the body.
- Colostomies are placed in the large intestine, or colon. They are lower down in the digestive system. Colostomies are typically on the right side of the body.
Each type of ostomy has a purpose, and the one that’s best for your particular needs will be determined by your surgeon. The part of the bowel that is below or ‘after’ the ostomy is referred to as the distal bowel.
What is an Ostomy reversal, or ‘take down’?
An ostomy reversal is a surgical procedure that reconnects the bowel so that waste once again passes through the digestive system normally rather than through a stoma into an ostomy bag.
Many ostomies are created temporarily during treatment for conditions such as:
- Colorectal cancer
- Diverticulitis
- Inflammatory bowel disease
- Traumatic bowel injury
- Intestinal blockage
- Surgical complications
Once the bowel has healed and your doctor determines it is safe, reversal surgery may be possible.
Important Advice
Learn all that you can about the procedure, your surgeon’s opinion of your prognosis and healing process, and what you can expect in the healing process, before your surgery. Don’t go into the process ‘blind’, but fully educated about what you can anticipate. This will prevent surprises.
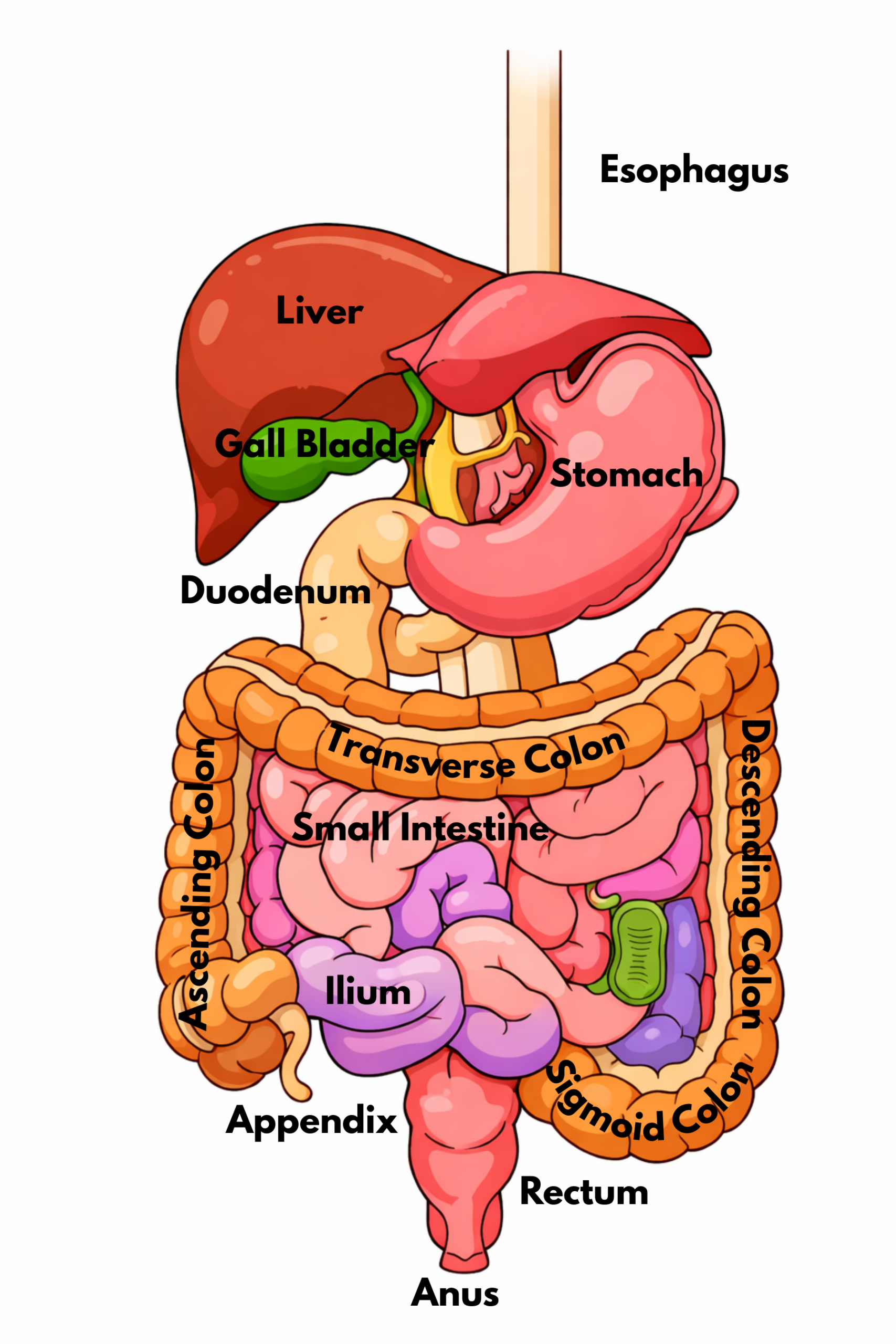
The Human Digestive Tract
The Process
It’s important to have a visual of the components of the digestive system to understand what’s involved with restoring the normal bowel pathway.
This diagram shows those components. When a person has an ileostomy or colostomy, this pathway is interrupted, and stool exits the body ‘early’ through that os, or opening.
Why is this visual important?
The portion of the bowel that is beneath the ostomy will be unused for a period of time. It basically ‘sits there’ with nothing much to do, and over time can become inflamed.
Where your ostomy was placed may be a factor in your healing process. An ileostomy is ‘earlier’ in the digestive tract, so more of the bowel will potentially be inflamed. A colostomy uses more of the bowel as it’s ‘later’ in the tract (think of it as lower down the pathway), so less of the bowel is unused.
This inflammation is called ‘disuse proctotis’. The degree to which the bowel is inflamed can play a large role in how easy or challenging recovery from surgery will be.
During reversal surgery, the surgeon reconnects the bowel internally, and closes the stoma. After recovery, digestion resumes through this pathway as it did before surgery.
However…
- Did your unique situation leave you without portions of your transverse or descending colon?
- Did you have radiation that may have damaged tissues like your rectum?
- Is your remaining bowel healthy, or do you have diverticulitis, ulcerative colitis, or Chrons?
- Was your ilium affected?
- Do you have your sigmoid colon, or part of it? This is the ‘holding tank’ of the bowel, and helps to prevent extreme urgency.
- Do you have all or part of your rectum, or was it removed?
- How long were you diverted?
The anatomical changes that have been made surgically can play a role in the recovery process.
Understanding the procedure and what to expect can help patients feel more prepared and confident when discussing options with their medical team.
IMPORTANT! Every, single person is unique!
There are many accounts of patients with no remaining rectum, no large intestine at all (their small intestine routes directly to their rectum), or other anatomical ‘challenges’ having entirely successful reversals.
It’s vital to understand that there are no guarantees in either direction:
- Some patients with highly compromised digestive tracts are reversed successfully and even return to normal function quickly.
- Some with few apparent complications develop Lower Anterior Resection Syndrome, or LARS.
It’s difficult to accurately predict the outcome, but the very, very good news is that the majority of stoma reversals are deemed a success. (Statistics vary, but most sources we researched quoted success rates between 80 and 95%, with success meaning that they never return to a bag and restore some degree of normal bowel function).
Am I a Candidate for Ostomy Reversal?
Not everyone with an ostomy will be eligible for reversal surgery, but many patients are.
Your surgeon will consider several factors when determining whether reversal is possible, including:
- The condition that created the need for an ostomy
- Whether the bowel has healed properly
- Your overall health and ability to tolerate surgery
- The health and function of the remaining bowel
- Any scar tissue or complications from previous operations
In some cases, reversal can be planned within a few months after the initial surgery. In other situations, doctors may recommend waiting longer to ensure healing is complete.
Patients often benefit from preparing questions for their surgeon, such as:
- Is my ostomy temporary or permanent?
- What tests determine whether reversal is possible?
- What risks apply to my specific situation?
- What kind of recovery should I expect?
Having these conversations early can help you understand the path ahead and make informed decisions about your care. The best path forward is to have these open, frank discussions with your surgeon. The worst path is to go into your surgery uninformed about the factors involved and the potential outcome.
The process of your take down will be determined by your surgeon and your particular health considerations.
If you have had a colostomy, it may be necessary to convert you to a temporary ileostomy for a period of time to allow your lower bowel to heal from surgery.
Be aware, in advance, if your surgeon feels that this interim step may be necessary – don’t let yourself be surprised when you wake up from surgery.
This step-wise take down process is common in the event of cancer; after tumor removal surgery, the large bowel may need time to heal. So, the waste will be diverted ‘higher up’ in the digestive tract through the use of an ileostomy, allowing the distal bowel to sit unused and for the surgical site to heal for a period of time before the complete reversal occurs.
This interim step is not atypical, and should be discussed with your surgeon as a possibility so you aren’t taken by surprise.